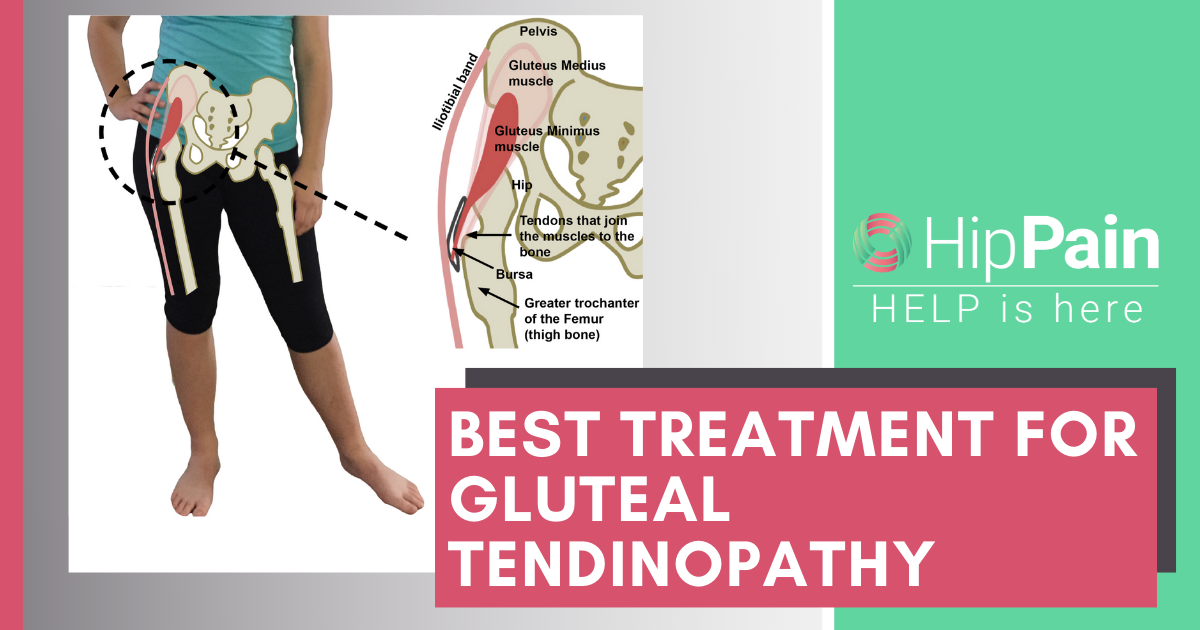
Gluteal Tendinopathy (or Trochanteric Bursitis) Diagnosis
Following a thorough interview and establishing that you have these gluteal tendinoapthy symptoms, there are a number of special tests that a health professional can perform in order to make a gluteal tendinopathy diagnosis (+/- trochanteric bursitis, GTPS). A couple of the tests that researchers have found most useful in diagnosing this condition1, you can perform at home yourself.
1. Sustained Single Leg Stance Test (Watch the video below)
Stand side on to a wall, with your sore hip furthest from the wall
Place 1 finger, from the nearside hand, on the wall at about shoulder height – this is just to help with balance
Now lift the nearside foot up behind you, just clearing the foot from the ground
Stand here for up to 30seconds
If you develop pain over the side of the hip within this 30 seconds, you may have gluteal tendinopathy.
(If you experience pain more quickly than 30seconds, don’t keep holding there, the test is positive)
Note: A positive test result significantly improves the chances that you have this problem. Some people will however test negative on this test and still have the problem, so this test is most useful for indicating a diagnosis of gluteal tendinopathy (+/- bursitis, GTPS) when it is positive1.