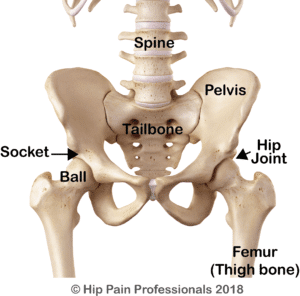
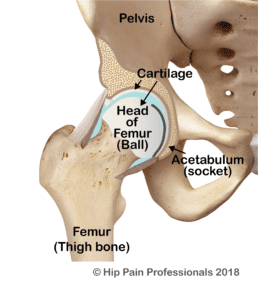
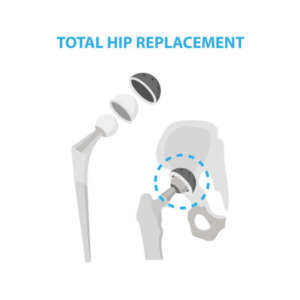
Hip osteoarthritis (OA) is a condition that makes the joint painful and stiff. Osteoarthritis is the most common form of arthritis. There are other forms of arthritis (that may be related to a systemic health condition), for example, Rheumatoid Arthritis, but here we will only discuss osteoarthritis. Treatment will be different, so it is always important to know what type of arthritis you have. Discuss this with your Hip Pain Professional. Here, we will only discuss osteoarthritis.