Pain deep in the buttock is often referred to in the literature as Deep Gluteal Syndrome. Other conditions that may be diagnosed in this area include Pirformis Syndrome and Sciatica. In this page we will discuss hip/pelvic related causes and treatment for pain in the area of the mid buttock.
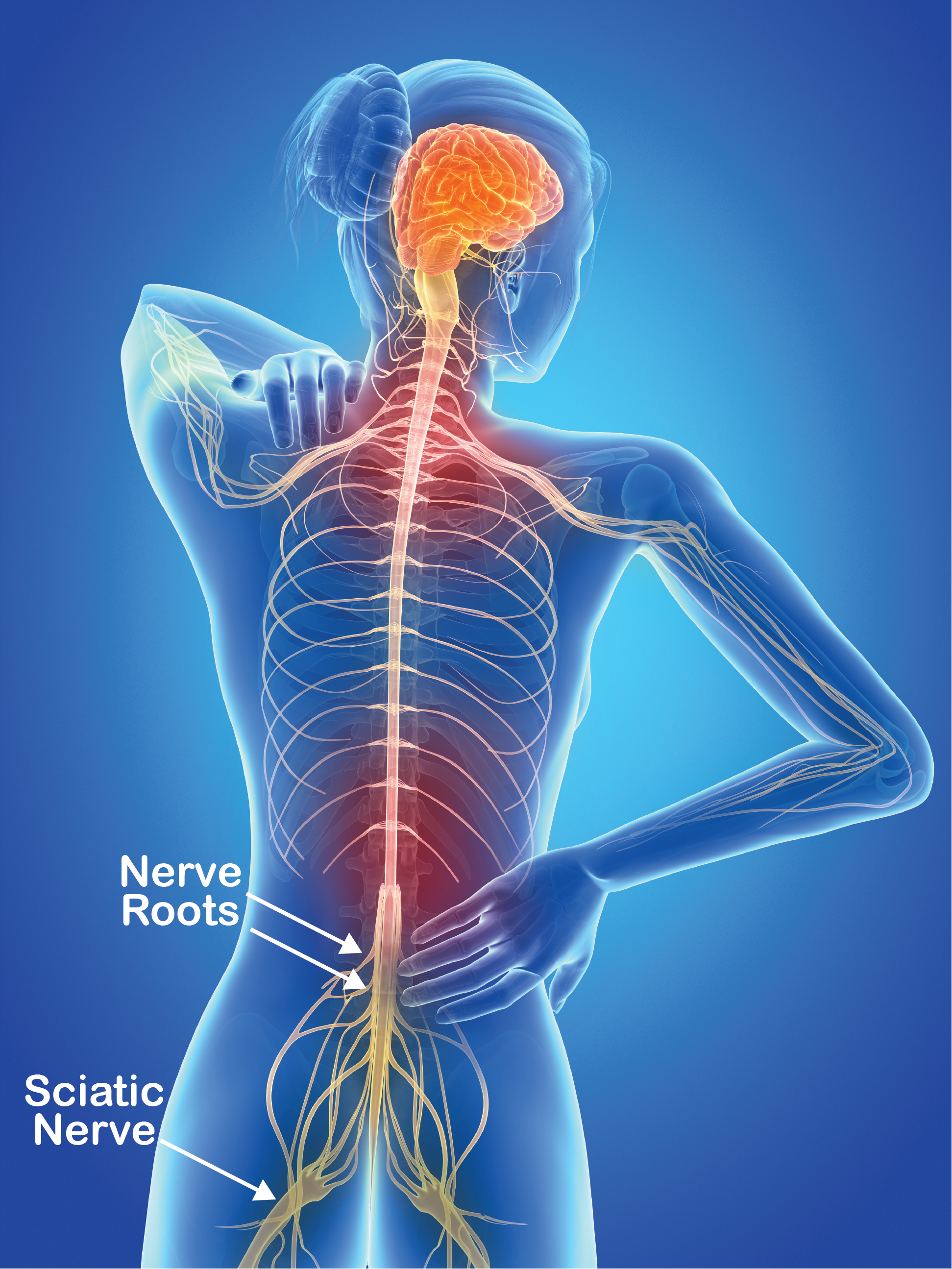
The term “sciatica” is often used incorrectly in reference to any pain felt in the area running from the back, down into the leg. Back-related nerve pain is more correctly referred to as radicular pain. Radicular pain is pain related to an irritation of the nerve roots as they exit the spine. Nerve roots (Figure 1) leave the spinal cord via the intervertebral foramina (holes or spaces between the vertebrae) and join together from various levels of the spine to travel as cord-like structures, called nerves, to their destinations. It is these nerves that travel outside the spinal cord that are referred to as “peripheral nerves”. Along their journey these peripheral nerves run between and through muscles and fibrous tunnels.
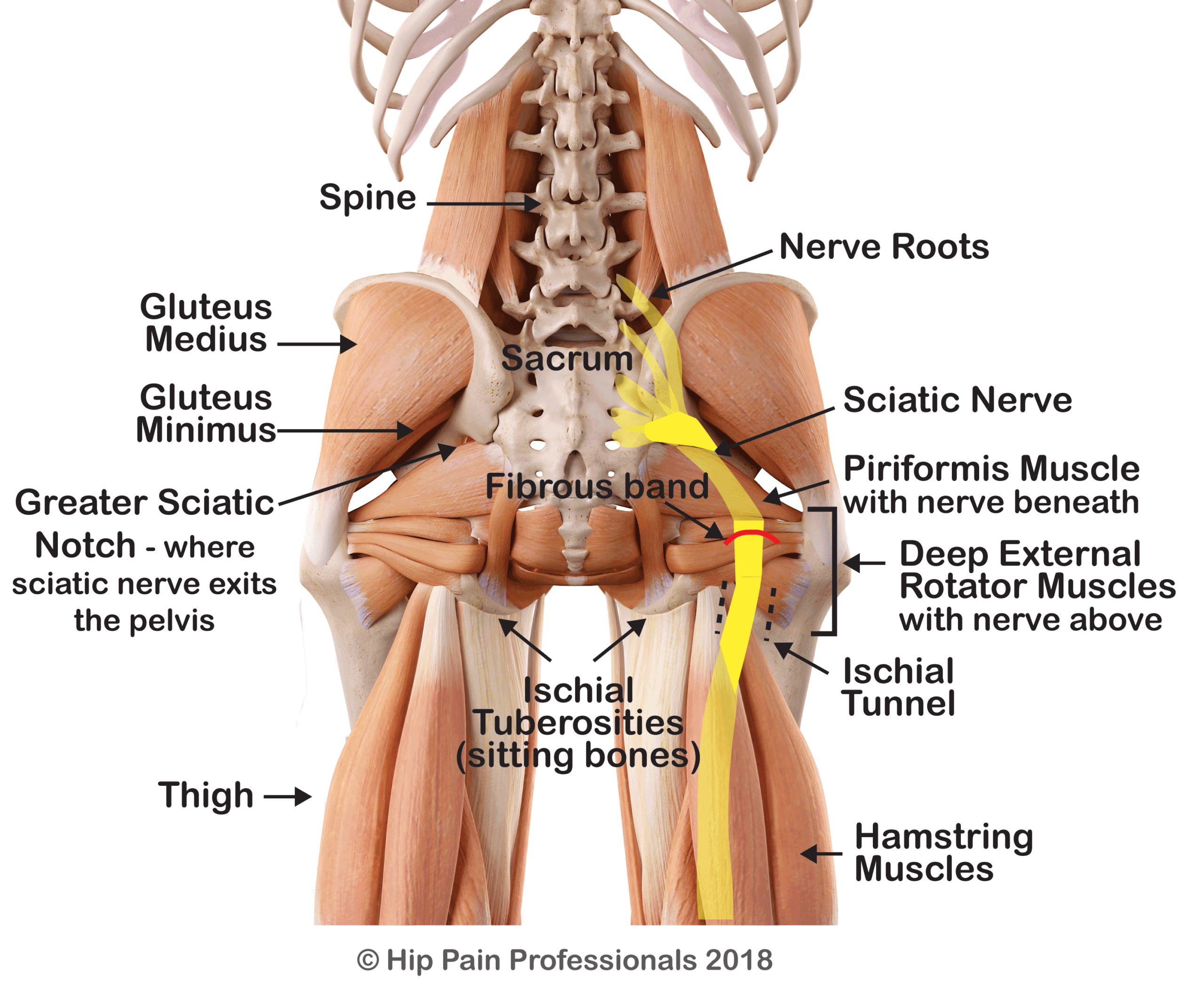
The sciatic nerve (Figure 1) is a peripheral nerve. While radicular pain arises from a problem as the nerve root exits the spine, nerve-related pain may develop due to a problem along the pathway of a peripheral nerve, outside the spine. Pain related to a nerve is called “Neuralgia” – which simply means nerve-pain. The term “sciatica” should be used to refer to neuralgia of the sciatic nerve. Here we will discuss sciatica associated with irritation of the nerve as it runs through the buttock, across the back of the hip.