
Pain is an experience that the brain creates for the purposes of stimulating you to change your behaviour or seek help for a perceived problem with your body. Irritating or potentially damaging stimuli in your body (like high levels of pressure, tension or extremes of temperature) activate sense receptors (danger sensors) in the area. Signals from danger sensors in the body travel through the nervous system to the brain. Here the information is processed and the brain sometimes (but not always) produces a pain experience.
These danger sensors send warning signals to your brain, and your brain then decides whether the signals are dangerous to your health. Your brain uses lots of other stored and real-time information to make this decision, for example:
After much scientific study, we now know that pain is not as simple as we once thought.
It has been clearly demonstrated that:
Pain is rather a reflection of how dangerous the brain perceives the situation to be and how important it thinks it is for you to do something about it, based on subconscious considerations.
The brain truly is amazing!
Persistent or cumulative signals from the danger sensors in your body, will usually trigger a pain experience, but at varying levels for each individual. Danger signals may come from many different structures around the hip and pelvis.
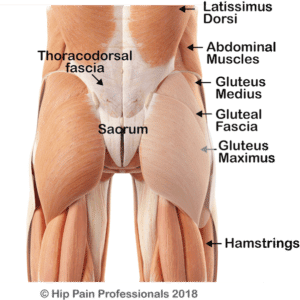
Figure 1: ‘Soft tissues’, non-bony structures, such as muscles and the tendons that attach them to.
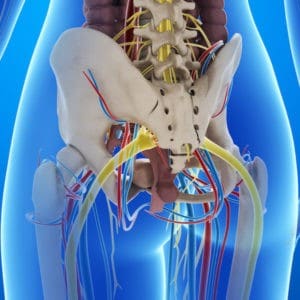
Figure 2: Nerves that run through and around the hip & pelvis. And pelvic organs or blood vessels, or other health issues masquerading as hip pain
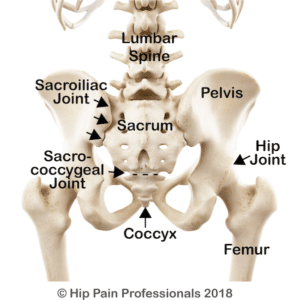
Figure 3: Bones and joints of the hip, pelvis and lower back
This blog was written by Dr. Alison Grimaldi, with contribution from one of our Hip Pain Professionals, Kirsty McNab, experienced physiotherapist.
Dr. Alison Grimaldi is a globally recognised expert physiotherapist, researcher, and educator, who has over 30 years professional clinical experience helping patients recover from a wide range of hip and pelvic conditions.

Dr. Alison Grimaldi BPhty, MPhty(Sports), PhD, FACP
Dr Grimaldi has completed Bachelor of Physiotherapy, Master of Physiotherapy and Doctor of Philosophy (Physiotherapy) degrees. She is a fellow of the Australian College of Physiotherapists, Practice Principal of PhysioTec Physiotherapy, an Australian Sports Physiotherapist , an Adjunct Senior Research Fellow at the University of Queensland, as well as an author and global educator. Her passion is helping people with hip pain, and educating other health professionals around how to help more people with hip pain.
Over the next few weeks we will be discussing all sort of different contributors to hip pain and things you can do to better understand and recover from these situations. Next week we will start by looking at the hip joint itself and the structures within the joint that may be involved with pain.
Remember a Hip Pain Professional can help you with a diagnosis and a recovery plan.

